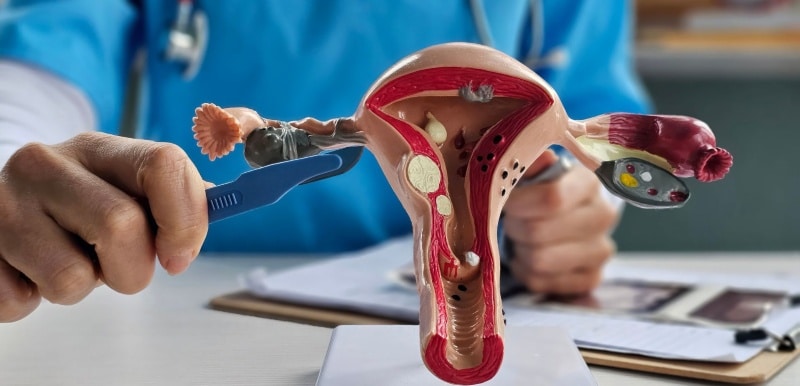
Finding out you have uterine fibroids can feel unsettling, especially when you’re unsure what comes next. These noncancerous growths form from muscle and connective tissue in the uterus, and while they’re common, they don’t always need treatment.
The real question is not whether fibroids exist, but whether they are actually affecting your health, comfort, or daily life. Understanding when treatment is recommended and when watchful waiting is enough helps you make confident, informed decisions.
How Common Are Fibroids?
Fibroids are far more widespread than many people realize. Research shows that up to 89% of women in their reproductive age develop uterine fibroids, making it the leading cause of hysterectomy in the US. That number alone can sound alarming, but it’s important to keep perspective. Many of these growths remain small, cause no symptoms, and are discovered incidentally during a routine pelvic exam or imaging for another reason.
The key takeaway is that prevalence does not equal severity. Most people with fibroids will never need fibroid surgery, and some may never even know they have them. Treatment decisions depend on symptoms, growth patterns, and personal goals such as fertility, not on diagnosis alone.
When Fibroids Start to Interfere With Daily Life?
Treatment is usually considered when fibroids cause noticeable or disruptive problems. Common fibroid-related symptoms include heavy menstrual bleeding, worsening menstrual blood loss, and anemia-related fatigue linked to excessive blood loss. In some cases, pressure effects lead to pelvic pain and discomfort, or urinary frequency if nearby organs are compressed.
A frequent challenge is uncertainty. You may notice changes in your cycle or increasing discomfort but struggle to connect them to fibroids. This is where proper evaluation matters. Imaging, such as transabdominal ultrasound or transvaginal ultrasound, helps determine fibroid volume and location, while lab tests, like a blood count, can reveal whether bleeding has affected your overall health.
In more complex cases, advanced methods such as magnetic resonance imaging or a Computed Tomography scan may be used, sometimes with contrast material, to better understand the uterus and surrounding structures. These details guide safer, more targeted care, especially when weighing different fibroid treatment options.
Specialized centers, including Dr TC Chang uterus fibroid treatment Singapore, often focus on individualized care plans. By matching symptoms with imaging findings and personal priorities, treatment can address the root cause without unnecessary intervention.
Situations Where Treatment May Not Be Needed
 Not every fibroid requires action. If your symptoms are mild, stable, or absent, observation may be the best choice. Small fibroids with minimal impact on uterine volume can often be monitored over time, especially if they are not affecting fertility or quality of life.
Not every fibroid requires action. If your symptoms are mild, stable, or absent, observation may be the best choice. Small fibroids with minimal impact on uterine volume can often be monitored over time, especially if they are not affecting fertility or quality of life.
Medical management is often the first step. Options may include the contraceptive pill, oral progestogen, tranexamic acid tablets, or a levonorgestrel intrauterine system to control bleeding. These approaches don’t remove fibroids, but they can significantly reduce symptoms while preserving bone mineral density and avoiding procedural risks.
When Procedures Become the Better Option?
When symptoms persist or worsen despite medication, minimally invasive procedures may be recommended. Treatments such as uterine artery embolization, also known as uterine fibroid embolization, work by blocking the fibroid’s blood supply using small particles delivered by an interventional radiologist trained in interventional radiology. Reduced circulation causes fibroids to shrink, easing symptoms without removing the uterus.
Other non-surgical options include focused ultrasound, where high-frequency sound waves target fibroids precisely. A more advanced form, magnetic resonance imaging or MRI-guided focused ultrasound, combines real-time imaging with energy delivery for accuracy. Thermal techniques like radiofrequency ablation and laparoscopic radiofrequency ablation destroy fibroid tissue directly while sparing surrounding areas.
Surgical approaches still have a role. Laparoscopic myomectomy, sometimes performed as a robotic procedure, is part of minimally invasive gynecologic surgery and may be preferred if preserving fertility is a priority. For specific bleeding issues, endometrial ablation may help, though it’s not suitable for everyone.
Recovery, Risks, and Long-Term Considerations
Any procedure carries potential adverse events and understanding them is part of good patient selection. For example, embolization may involve post-embolization syndrome, which can include temporary pain, fever, or fatigue. Recovery guidance often emphasizes pacing yourself and learning to stay active post-surgery, favoring light movements over vigorous exercise to support healing without strain.
Follow-up care is equally critical to the procedure itself. Monitoring symptoms, reassessing imaging, and checking lab values help ensure that treatment goals are met. If symptoms return or change, it’s wise to make an appointment promptly to reassess next steps.
A Thoughtful Path Forward
Deciding whether to treat fibroids isn’t about choosing the most aggressive option—it’s about choosing the right one for you. Some people thrive with simple monitoring, while others benefit from targeted procedures that relieve symptoms and restore comfort. By understanding when treatment is recommended and when it’s not, you place yourself at the center of the decision-making process, supported by evidence, expertise, and your own priorities.